Maryjo L. Cleveland, MD
Medical Director, Post Acute & Senior Services
Chief, Division of Geriatric Medicine
Summa Health System
Akron, Ohio
There are many issues facing older adults that are common, but should not be considered inevitable. This blog will launch a series for 2014, all bundled under the general heading of “It’s Not Normal”. Over the next year, I intend to cover a variety of topics that include dementia, incontinence, falls and depression. If you have suggestions for this series, please leave a comment.
The kick-off for this series is pain. While pain is common as we age, it should never be considered “normal”. Pain should always be discussed with your healthcare provider, so that he or she can help determine the cause (or causes). Your healthcare provider can then help you figure out an approach to remove or reduce both the pain and the affect it has on your life.
Acute pain is pain that has happened recently and usually has a known cause. An example of this is a sprained ankle. A few weeks of ice, rest and over the counter pain medications (such as acetaminophen) is usually all that is required for relief to occur.
Chronic or persistent pain, however, is more of a problem. You may have had this pain for some time and the direct cause may not be known. There are different kinds of chronic pain. These include:
- pain from nerves, such as diabetic neuropathy or pain from a stroke
- joint or bone pain such as arthritis or gout
- some kinds of internal pain, such as abdominal pain from Irritable Bowel Syndrome
Managing your persistent pain requires telling your healthcare provider a complete history, including how much pain you have, what makes the pain better or worse, and what the pain feels like.. Some pain is very hard to describe. Be sure that your health care provider understands as best as possible, what it feels like to you. Words like “burning”, “aching” or “stabbing” will help guide our evaluation and treatment.
In Geriatric Medicine, we are very concerned about how your condition affects your quality of life. We will want to know if your pain affects your ability to do the things you love. Pain can worsen your sleep, prevent you from exercising and cause depression. In fact, this can be looked at as a classic “vicious cycle”.
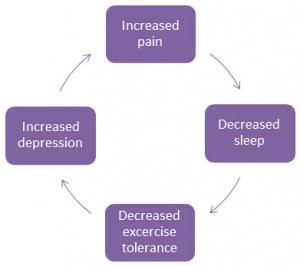 It is important that the cycle is interrupted in at least 2 spots. Medicine that reduces pain is important but it is also just as important to consider other approaches as well:
It is important that the cycle is interrupted in at least 2 spots. Medicine that reduces pain is important but it is also just as important to consider other approaches as well:
- Sleep – adopt better sleeping habits that include reducing caffeine, using a dark room and taking pain medications before bed.
- Activity – physical therapy can help to reduce pain, but so can daily exercise!
- Depression – if your mood is affected, it is important to focus on this with counseling and/or medications.
If you are dealing with chronic pain, learn more by reviewing the Guide to Medications for Persistent Pain and be sure to see your healthcare provider as soon as you can. Because no one should live with pain. Remember, it’s Not Normal!

